The Gut Brain Connection

Ever heard of the phrase ‘gut feeling’ or felt the ‘butterflies’ in your stomach? These experiences can be explained by the gut-brain axis, the communication network that connects the brain and gut, physically and biochemically. This may seem like a minor thing, right? That is until you realise it’s essentially like our ‘second brain’. Yup you read that right! Who knew that hidden in our digestive system are two thin layers of over 100 million nerve cells that dutifully line our intestine all the way from gullet to rectum. They make up what is known as the enteric nervous system (ENS).
Let’s see how our ‘second brain’ interacts with the rest of our body!
How Gut Health Affects Our Body
Are you wondering how on earth your brain directly connects to your gut? The answer is simple (unlike the many complex tasks it carries out)! The Vagus nerve is an important two way connector between the brain and gut. It’s found to play a crucial role in our thoughts, feelings and behaviours.
Stress is noted to inhibit the signals along this nerve causing intestinal distress. You may experience this phenomenon more often if you suffer from pesky IBS (Irritable Bowel Syndrome) as it reduces Vagus nerve function.
Alternatively, do you ever find yourself battling against big emotional shifts like heightened or irrational fear, anxiety and stress? This may be triggered by your ENS. So if you suffer from IBS or any other functional bowel problems, you have a higher chance of being diagnosed with psychological disorders like depression and anxiety because of this connection resulting in poorer mental health!
Neurotransmitters are chemicals that control feelings and emotions. These are mainly produced in the brain but also by our gut cells and the trillions of microbes that live there! For example, a large proportion of the serotonin neurotransmitter associated with happy feelings is produced in the gut. Gut microbes also make the GABA neurotransmitter, which helps control fear and anxiety.
It’s important to note that these chemicals released by gut microbes also affect brain function. So preserving our ‘second brain’ will eventually support our real brain! Poor gut health results in the microbes releasing lipopolysaccharide (LPS), an inflammatory toxin made by certain bacteria that enters the bloodstream and causes inflammation especially in those with higher intestinal permeability. Inflammation and high LPS in the blood have been associated with a number of brain disorders including severe depression, dementia and schizophrenia.

Consequences Of Ignoring Gut Health
Your gut is a giant chemical factory that helps you digest food, regulate hormones and produce healing compounds to keep your entire body healthy. When the gut starts to break down, it won’t be long before the rest of your body starts to break down too!
Imagine this, you’re building a house and for the foundation you carefully lay bricks and cement it all together to protect its inhabitants from the dangers outside. Now, transferring this analogy, our own intestinal wall has to be intact to prevent the passage of dangerous toxins, pathogens, and other proinflammatory substances into the human body. If it fails to do so and is more ‘naive and friendly’ it will let these enemies permeate our defence lines and wage war on us! This may result in system wide inflammation and cause disease.
The ‘leaky gut hypothesis’ explains that poor intestinal barrier function may induce chronic inflammatory changes in the target organs by virtue of those little microbial products produced in the gut that cross over into the body.
Just like a poor foundation will result in a house that will crumble, poor intestine health and its increased permeability have been found in many diseases like inflammatory bowel disease (IBD), irritable bowel syndrome, type 1 and type 2 diabetes, depression, and more.
Foods That Will Better Your Gut Health
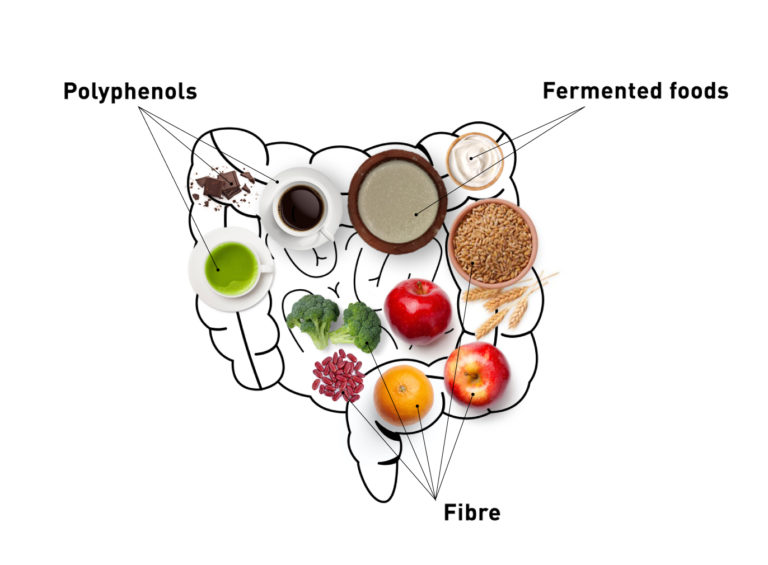
Eating a diverse range of foods will result in, you guessed it, a diverse microbiome!
- Up the fibre: In particular, legumes, whole grains, beans and fresh fruit which contain lots of fibre and can promote the growth of healthy bacteria which then helps digest fibre, produce important chemicals like B vitamins and prevent infections from other bacteria like E. coli. The fibre feeds your gut microbes and helps them do their job, which is to protect you! Remember apart from being fibre rich, these plant-based foods are also great sources of other longevity-supporting nutrients, like antioxidants which are known to prevent chronic inflammation.
- Eat. Fermented. Foods! They contain healthy bacteria and can reduce the number of disease-causing species in the gut. These foods include yoghurt, curd, tofu and miso paste. Who knew such sour foods could be so sweet to our body!
- You’ve heard of probiotics but what about prebiotics? They are different from probiotics in that they promote the growth of healthy bacteria in your gut whilst probiotics either consumed as a supplement or found in naturally fermented foods are live bacteria that can help restore the gut to a healthy state after dysbiosis, which happens when gut bacteria become an unbalanced. Prebiotic rich food includes artichokes, bananas, asparagus, oats and apples.
4. Eat polyphenol rich foods! These plant compounds are found in red wine, green tea, dark chocolate, coffee and whole grains. These foods contain plenty of antioxidants and also help your gut find the good bacteria army!
5. Do you often crave that sugar ‘high’? Do you ‘inhale’ those delicious sweets when you’re feeling stressed or when you feel … wait, I mean who needs an excuse to eat sweets anyways! We all just eat sweets because they’re such a treat! These days however pretty much everyone has heard the diet craze of cutting out refined sugar BUT some people often mistranslated this to EAT ARTIFICAL SWEETNERS. Hmmm … raise your hands if you’ve done this! Artificial sweeteners have been linked to increasing the growth of unhealthy bacteria in the gut microbiome.
6. When you think of the word antibiotics, you think it’s a miracle cure to your infections. But think of antibiotics like a hyperactive child. This child will love to play with all the toys in the room, just like your antibiotics fighting off bad bacteria in the body, but this kid will play with the room’s furniture even though it’s not meant to be played with. Just like that, antibiotics may also fight off your good bacteria too. So, use it only when necessary!
If you have any concerns regarding your gut health, you can speak to a doctor via the oDoc app from the comfort and privacy of your home. GPs and Specialised doctors like gastroenterologists are also available to consult.
Download oDoc today on the App Store or Play store.
References
- The Brain-Gut Connection, Johns Hopkins (2022)
- Gut Health and Pain – Part 3: Your Gut and Stress, Northern Pain Centre (2021)
- The Gut-Brain Connection: How it Works and The Role of Nutrition, Healthline (2020)
- Increased Intestinal Permeability and Decreased Barrier Function: Does It Really Influence the Risk of Inflammation?, NCBI (2016)
- Here’s How the Longest-Living People on the Planet Maintain Optimal Gut Health, Well + Good (2022)
Similar Articles...

Let’s talk flu, its prevention and home remedies.
Boo-ger season is here! Let’s begin by defining flu (short term for influenza) because it’s usually misunderstood as fever or cold. Flu is a common

Menopause Brain Fog is real: A Simple Guide with Symptoms and Treatment
Menopause Brain Fog is real: A Simple Guide with Symptoms and Treatment Women in their 40s and 50s who are just entering the end of

How to Keep Work Stress from Taking Over Your Life
How to Keep Work Stress from Taking Over Your Life In today’s fast-paced and competitive world, work stress has become an all-too-common problem that affects
