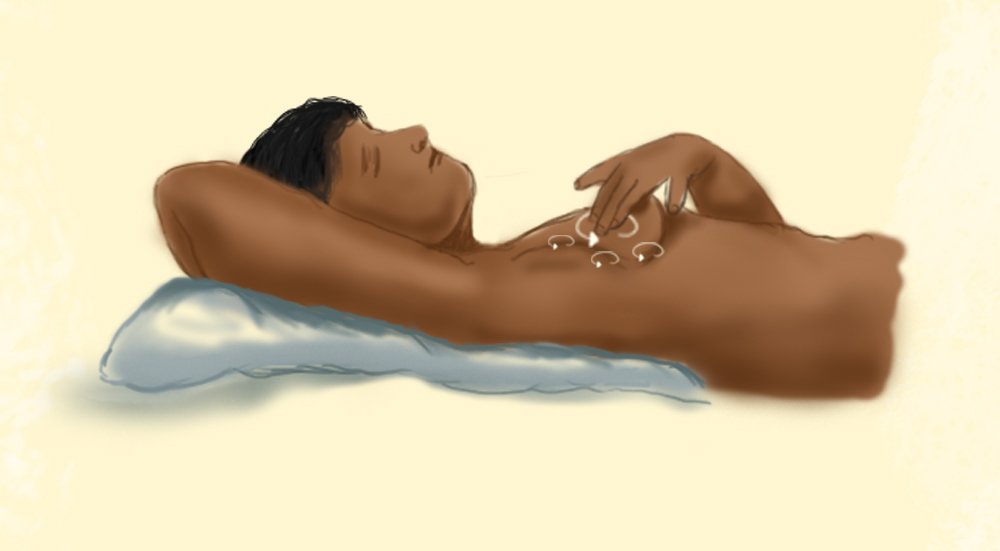
4. Feel your breasts in the same manner whilst you are standing or sitting. This is ideally done in the shower as the water and soap allow for a smoother movement.
What to do if you discover a lump or any visible changes
Do not panic. Not all breast lumps or bumps mean breast cancer. In fact, most turn out to be benign (non-cancerous). Non-cancerous breast lumps can be caused by hormonal changes, injuries or a benign condition. However, it is vital that all bumps are discussed with a medical professional.
Don’t be shy, speak to a medical professional. Early detection does save lives. So if you have noticed a lump lasting for longer than one menstrual cycle, it’s important to speak to a family doctor or a GP. The doctor will most often refer you to an imaging test. Ultrasounds are often the only test used for women under 30 whilst ultrasound and mammograms are used for women over 30.
Do ask questions. Here are a few you can ask your GP to help you gain clarity.
- What tests are needed to find out if the lump is cancerous?
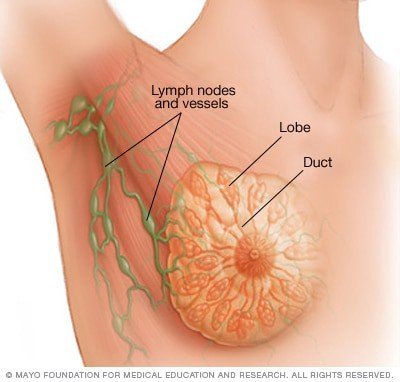
- In addition to a physical exam of my breasts, will you check the lymph nodes in my armpits and neck?
- Should I get a mammogram?
- Will I need a biopsy?
- What does a biopsy involve?
- How long will it take to get the results?
- If the tests are negative but the lump is still there, what are the next steps?
- If the tests are clear and the lump goes away, how often should I follow up with you?
If unsatisfied with answers or level of care, do get a second opinion.
How often should I perform a breast self-exam?
Do it every month around 7-10 days after your period starts. This is when your breasts are as tender or lumpy and make sure to examine them before you start menstruating as well. Therefore, you can understand the natural changes.
If you are no longer menstruating, do it at regular intervals every month.
In both instances, make sure to journal the changes with date
What are the risk factors?
Risk factors are aspects that make it more likely that someone could develop breast cancer, however, having one or a combination of these factors doesn’t mean you’ll get it. A healthy awareness of risk factors will allow you to take steps to mitigate the risk.
- Gender: women are more likely than men to develop breast cancer
- Age: incidence of breast cancer increases with age
- Personal history of breast conditions or breast cancer: if you have developed breast cancer in one breast, there is a higher risk of developing it on the other.
- Family history of breast cancer: if a close female relative has experienced breast cancer, there is an increased risk however in most diagnosed patients, there is no family history of breast cancer
- Genetic predisposition: the most well-known gene mutations are the BRCA1 and BRCA2 and can be passed from parents to children. Though these genes can greatly increase the risk, it is not inevitable.
- Obesity
- Alcohol intake
- Postmenopausal hormonal therapy: whilst women are on hormone replacement medications, they have an increased risk. However, once they stop the medications, this risk declines.
- Beginning your period at an age younger than 12
- Beginning your menopause at an older age
- Having never been pregnant
- Having your first child at an age older than 30
How can I reduce my risk of breast cancer?
Whilst there are no hard and fast rules on ensuring one doesn’t develop breast cancer, the following non-exhaustive list is to help you mitigate your risk:
- Regular self-exams
- Consuming alcohol in moderation
- Exercising at least 30 minutes four times a week
- Maintaining a healthy weight
- Consuming a healthy, balanced, sustainable diet
- Limiting postmenopausal hormone therapy
- Limit exposure to radiation
When it comes to breast cancer, early detection does help save lives.
Make sure to carry out your self-examination, consult your doctor regularly and live a healthy life. Ignorance is usually bliss, just not here.
In 2022, Breast Cancer Awareness month focuses on the disparity of resources to fight this disease across the globe. If you are looking to take the first step, we are here
If you’d like to speak with a GP or a family doctor to discuss your questions or concerns, our oDoc partner doctors are available. Download oDoc here to get started.
Sources
- Breast Self-Exam, Breastcancer.org (2022)
- What Is Breast Cancer?, CDC (2022)
- Breast cancer, Mayo Clinic